Replacing IU Health Plans: What Small Groups Need to Know

If your small business has been using IU Health Plans for group health insurance, you might already know about Anthem’s recent purchase of IU Health Plans. Because of this, IU Health Plans will not renew small-group policies in 2025. For many small businesses, this creates stress and worry—especially if you have employees who have ongoing […]
2024 Employee Benefits Survey: Key Insurance Trends for Employers

The 2024 SHRM Employee Benefits Survey highlights critical trends in employer-sponsored insurance benefits, emphasizing the growing importance of health, dental, vision, and specialty coverage in today’s workforce. As employee expectations evolve, businesses must stay competitive by offering comprehensive Indiana Health Insurance solutions. Key Findings on Employer-Sponsored Insurance Benefits 1. Health Insurance Coverage Remains a Top […]
2025 Drug Copays

One of the health insurance trends we see across all carriers is the increased cost of drug copays. Almost every plane has moved to a Tier 2 Copay of $50. For the last decade, tier 2 has averaged around $35-$40. When you look into health insurance, you’ll quickly realize that prescription drug tiers matter. Drug […]
A Guide to Indiana Group Health Insurance Renewals for Employers

Navigating the Indiana Group Health Insurance renewal process can feel overwhelming, especially with the rising costs and maintaining quality coverage for your employees. Tips on Navigating Group Health Insurance 1. Start Early: Renewal Timeline The renewal process typically starts 60 to 90 days before plans renew. This window gives you enough time to review your […]
IU Health Plans to be Acquired by Anthem

IU Health Plans is a local insurance company owned by Indiana University Health, a non-profit healthcare system. IU Health Plans launched in 2013, offering health insurance plans to individuals, families, and employers. IU Health had a short run with Individual health insurance plans through the ACA. They offered competitive plans with rich coverage. However, IU […]
Indiana Hospitals Rank #8 as Most Expensive in the Country

A recent study by the Rand Corporation (https://www.rand.org/pubs/research_reports/RRA1144-2.html) Hoosiers Pay More Than Three Times the Medicare Reimbursement Rate for Health Care The Rand study, conducted from 2020 to 2022, is a comprehensive analysis of medical claims data from a diverse population of privately insured individuals and hospitals across the United States. This study’s findings, which […]
GLP-1s will no longer be available through Caremark Mail Service

CVS Caremark is a pharmacy benefit manager (PBM) and a third-party administrator of prescription drug programs. PBMs are primarily responsible for processing and paying prescription drug claims, negotiating discounts and rebates with drug manufacturers, and managing pharmacy networks for health insurance plans, employers, and government programs. CVS Caremark has over 100 million members who utilize […]
Navigating The Death of an Employee

Managing grief in any setting is a profoundly personal experience that doesn’t follow a set timeline or pattern. As an owner/HR/manager, supporting your team through a loss can be challenging but crucial for maintaining a healthy and compassionate work environment. Here’s a comprehensive guide on what to expect and how to navigate the grieving process […]
New Digital Insurance Cards

As we enter 2024, the health insurance and employee benefits industries are transitioning to digital ID cards. Traditional ID cards will be a thing of the past. The Insurance companies are adopting digital ID cards for several reasons, including: Cost Reduction: Producing physical ID cards involves printing, packaging, and mailing expenses. Convenience for Customers: Digital […]
Primary Care Physician Shortages
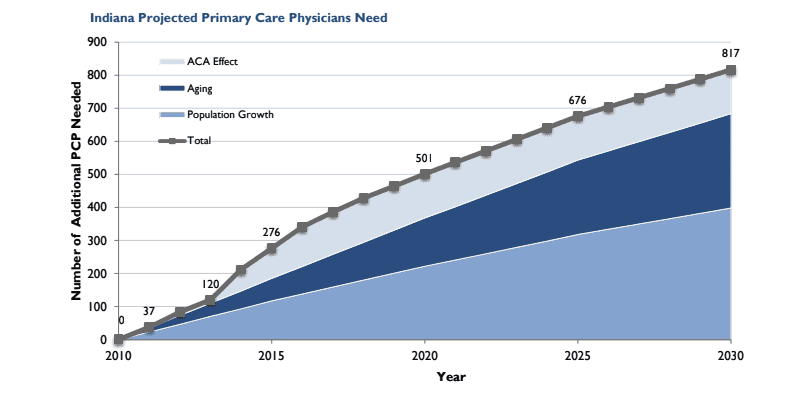
Primary care physician shortage is a significant concern in Indiana and the entire country. The average wait for an onsite appointment with a physician is 26 days, and that is in metropolitan areas. If you live in a rural community, it could be months. Several factors contribute to this shortage of Primary Care Doctors. Aging […]
