Trump Admin. Releases Final Rule on Short-Term Health Insurance

Short Term Health Insurance Final Rule 36 months of coverage Short-term health insurance is a policy that is very similar to pre-affordable care act coverage. The plan does not cover preexisting conditions and requires underwriting. If your accepted, the cost is 50%-60% less than an ACA product. These plans are also using traditional PPO networks, […]
Indiana Association Health Plans (AHPs)

The Department of Labor released their final rule on the creations of Association Health plans. There has been a great deal of criticism and misinformation in the media. The DOL final rules provide the guideline for setting up association health plans. These plans would be governed by both State and Federal guidelines. The Employee […]
2019 Individual Health Insurance for Indiana

The remaining two individual health insurance companies participating in the Indiana market have filed their rate for 2019. We now have two insurance companies offering personal health in 2019. CareSource and Celtic Insurance Company aka AM Better The good news is these two companies have decided to continue to offer individual health insurance coverage to […]
Anthem Buying Home Healthcare Aspire

Insurer Anthem Strikes Deal for Palliative Care Company Aspire Health Here is a story that was given very little media attention but is big news for Indiana’s Anthem. Anthem is buying Aspire Health that provides home healthcare services for patients suffering from serious illnesses. Aspires help patients and family manages symptoms of extreme illness to […]
Channel 13 Short Term Insurance Story

Channel 13 WTHR Investigates recently reported on a controversial story about Short-Term Health insurance and asked me to be a part of it being a health care professional. The story is about a family that had been using short-term health insurance and the woman was diagnosed with breast cancer. The policy she had purchased was […]
Tony Nefouse’s Complete Guide to Group Insurance: “Networks”

We come to the point where you are ready to start reviewing group insurance proposals. Before you start receiving insurance proposals information about your company should be taken into consideration. Employee location has a large impact on what type of plans a company should be entertain. Does the employer have employees in other states, does […]
Tony Nefouse’s Complete Guide to Group Insurance: Request for Proposal

At this point, you are ready to start submitting proposals for group insurance. First-year Benefit Offering: If you are offering a group health plan for the very first time, there are multiple issues to be aware of. Hopefully, you have surveyed the current employees and know who is interested in electing coverage. As the owner, […]
The Trumps Administration Blueprint to Lower Drug Prices
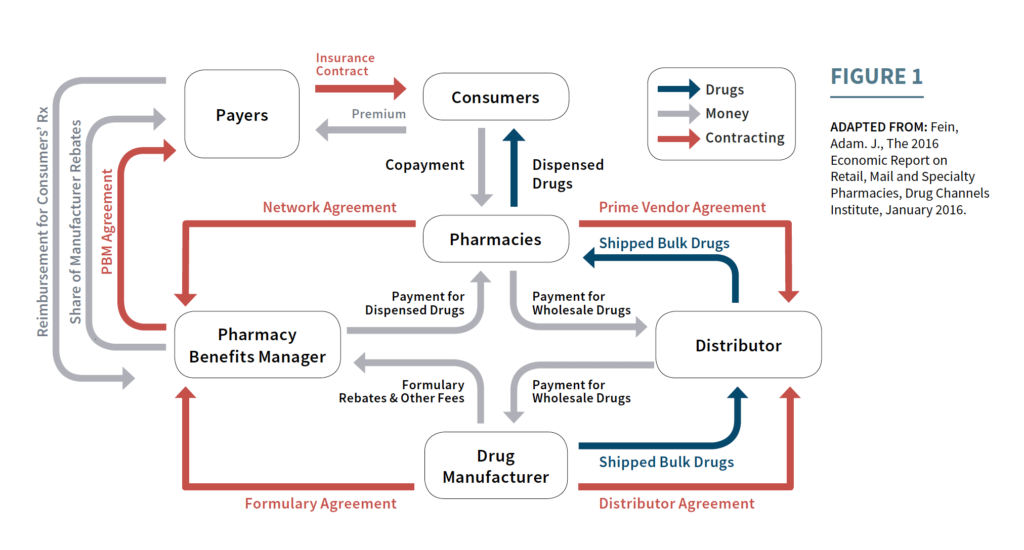
The Trump administration released the American Patient First which is a guide to lower drug prices. The blueprint provides two phases; Phase 1 is actions the President can take to lower prices, Phase 2 is for HHS actions of consideration and solicit feedback. The blueprint is looking at four areas to address, Increased Competition, Better […]
Tony Nefouse’s Complete Guide to Group Insurance: Obtaining A Quote
Obtaining proposals for group insurance benefits can be relatively easy. There are multiple outlets for receiving bids. Most of the insurance companies have now set up in-house sales; this allows groups to go direct to the carrier to obtain a proposal. Some payroll companies have broker divisions in which they can provide suggestions. The best […]
Tony Nefouse’s Complete Guide to Group Insurance

Many companies will turn to the internet to search for insurance benefits. Since 1998, we have been helping these businesses obtain group benefits. In the beginning of the internet, very few people would go to the world wide web for insurance information. Today that has all changed, business owners want information at their fingertips. We […]
